Brain cancer has left Tayden Ybarra, 16, legally blind in her left eye, says her…
Tag: WebMD
U.S. statistics hold an alarming disparity: Americans of East Asian descent face unusually high risks for stomach cancer
It happens quickly: A child on the autism spectrum bolts from supervision and disappears –…
The calls kept coming into the National Runaway Safeline during the pandemic: the desperate kids…
Heather Martin and her choir classmates were doing vocal warmups at Columbine High School on…
When police psychologists and law enforcement talk among themselves, they often conclude the same thing:…
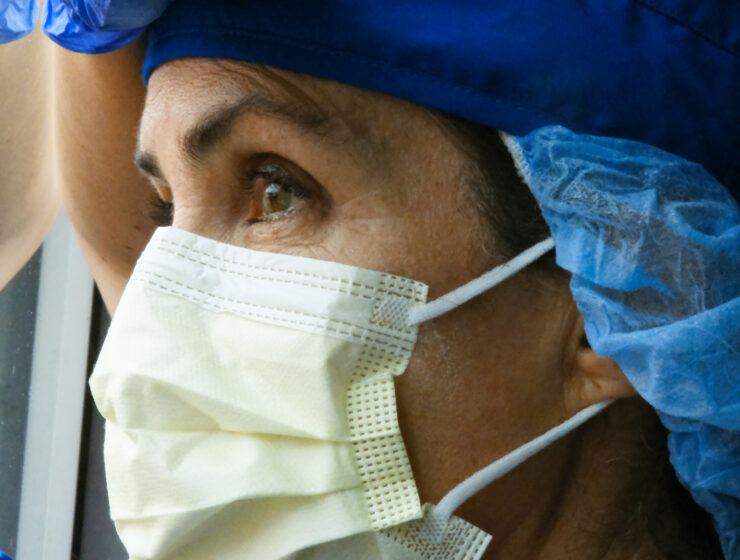
In 2 years of working as an emergency nurse at a hospital in the San…
During a second-grade Zoom class in Orange County, CA, a boy said, “I don’t like China or Chinese people…”
Sleep expert Rachel Manber, PhD, has seen the pervasive miseries of insomnia. Patients who are frustrated and fatigued tell her that they toss in bed all night, seeking that elusive comfortable spot. Others give up evening outings or vacations to avoid messing up their sleep schedules. Still others get anxious at bedtime, pondering whether to take sleep medications or wind down with a nightcap.
A young black doctor in training tweeted about disturbing incidents at his hospital. Samuel Kebede,…